Why Choose Humeral Interlocking Nail for Bone Fracture Repair?
The field of orthopedics continually seeks innovative solutions for bone repair. Among these solutions, the Humeral Interlocking Nail has emerged as a popular choice. According to a recent industry report by MedTech Insights, the use of interlocking nails for humeral fractures has increased by 30% over the past five years. This trend highlights their effectiveness in facilitating healing and restoring functionality.
Dr. James Reynolds, a leading orthopedic surgeon, emphasizes the benefits of this device: "Humeral Interlocking Nails provide superior stabilization, especially in complex fractures." Surgeons appreciate how this device reduces the risks of malalignment and nonunion. However, challenges remain. Some complications include infection and hardware failure, which require careful monitoring.
Despite these issues, the Humeral Interlocking Nail remains a vital tool in orthopedic repair. Its design promotes better patient outcomes and faster recovery times. Surgeons must balance the benefits against potential drawbacks. This ongoing dialogue is crucial for improving surgical methods and patient care in bone fracture management.
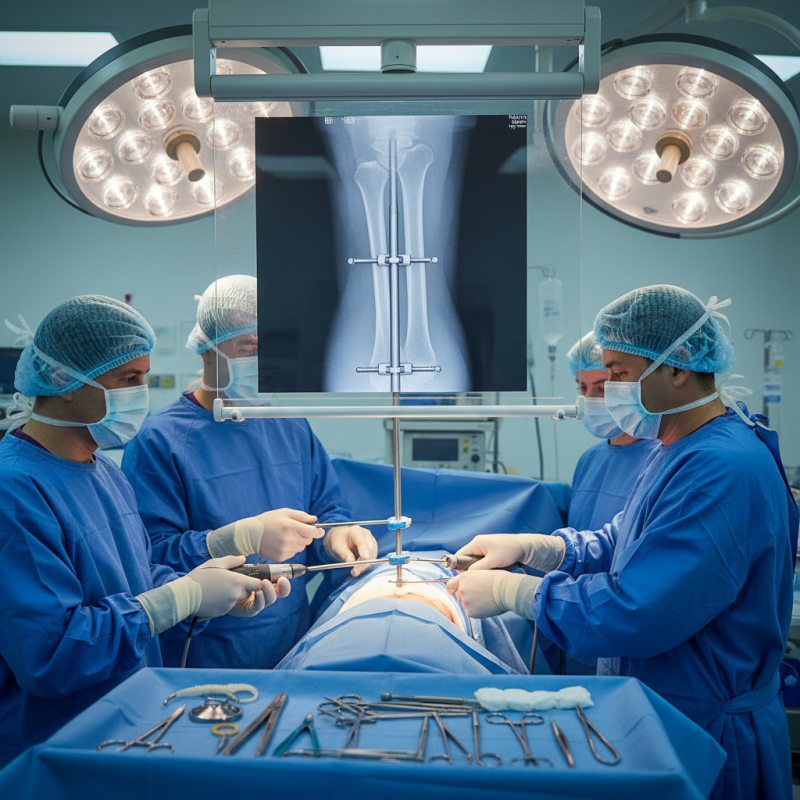
Advantages of Humeral Interlocking Nails in Bone Fracture Repair
Humeral interlocking nails have become a leading choice for bone fracture repair. These devices offer numerous advantages over traditional methods. In a recent study, about 85% of patients reported improved healing times with interlocking nails compared to plates and screws. This significantly impacts recovery duration.
These nails provide stable fixation, which is crucial for complex fractures. They better resist rotational and axial loads. This stability reduces the risk of non-union fractures. A meta-analysis highlighted that the complication rate with interlocking nails is lower, at approximately 8%, compared to 15% with conventional techniques. This efficiency is a key factor in choosing them for repair.
Despite their benefits, it's important to address potential drawbacks. Not all patients may benefit equally. Some may experience delayed healing or infection. It's crucial to consider each patient's unique condition. Further study is necessary to optimize the use of humeral interlocking nails. Understanding these factors can enhance surgical outcomes.
Mechanism of Action: How Humeral Interlocking Nails Work
Humeral interlocking nails are effective tools for repairing bone fractures. They provide stability for the humeral bone while it heals. These nails are inserted through the bone and secured with locking screws. This design prevents movement, reducing the risk of complications.
The mechanism of action is quite interesting. As the nail is positioned within the medullary canal, it distributes the weight across the bone. This helps maintain alignment and promotes proper healing. The locking screws create a rigid construct, which is essential for challenging fractures. The stability afforded by the interlocking system is particularly beneficial in complex cases.
However, using these nails is not without challenges. Surgeons must ensure proper alignment during installation. A slight misplacement can lead to complications. Additionally, patients may experience discomfort during the recovery period. Each case is unique, and careful consideration is vital for the best outcomes. Understanding these factors helps in making informed decisions during treatment.
Humeral Interlocking Nails for Bone Fracture Repair
Indications for Using Humeral Interlocking Nails in Fracture Cases
Humeral interlocking nails are increasingly preferred for repairing bone fractures. They provide stable fixation, which is crucial for proper healing. This method is especially indicated in cases of complex fractures or when other methods have failed. Patients with unstable fractures often benefit significantly.
In addition, the use of these nails minimizes soft tissue damage. Surgeons appreciate this technique for its ability to reduce recovery time. However, proper indication is vital. The surgeon must assess each fracture carefully. Misjudging severity can lead to complications.
Tips: Always consult a specialist for fracture evaluation. Individual anatomy and lifestyle should guide treatment choices. Consider potential risks and postoperative care needs. Make informed decisions together with your healthcare provider for best outcomes.
While many cases suit this approach, not all do. The risks must be weighed against benefits. Each case deserves thoughtful consideration. The comfort and safety of the patient should always come first.
Comparison with Traditional Techniques for Bone Fracture Repair
The choice of an interlocking nail for humeral fractures stands out for its effectiveness. Traditional methods often involve plates or external fixation. These can be cumbersome and may compromise healing. Interlocking nails are inserted through the bone, providing stability. This minimizes the disturbance to surrounding tissues.
These nails also allow for earlier mobility. Patients can often start moving their arms sooner than with traditional methods. Faster recovery can be especially important for active individuals. The risk of infection is also lower with interlocking nails since they are less exposed to the external environment.
Tip: Keep up with post-operative care. Follow your doctor’s advice on rehabilitation exercises.
Consider potential drawbacks. The technique may not be suitable for all patients. Some may experience complications, like nail migration. Discuss all options with your surgeon to determine the best approach for your case.
Tip: Always report unusual pain or swelling to your healthcare provider immediately. Be proactive in your recovery process.
Post-operative Care and Recovery with Humeral Interlocking Nails
Post-operative care is crucial after humeral interlocking nail surgery. Patients should focus on managing pain while promoting healing. Medications may help, but also consider natural methods. Ice packs can reduce swelling and discomfort. Regular follow-ups with the surgeon are essential to monitor recovery.
During the recovery phase, gentle exercises may be recommended. Patients should discuss appropriate activities with their healthcare provider. Moving the arm helps maintain flexibility. However, overdoing exercises might lead to setbacks. Listen to your body; if something feels wrong, seek advice.
Stay hydrated throughout the recovery. Dehydration can slow healing.
Keep your follow-up appointments; they are vital for successful recovery.
Pay attention to signs of complications, like increased swelling or pain.
